
8 steps to a successful ‘digital front door’ for healthcare styles-text-white
<p><br> January 09, 2023</p>
8 steps to a successful ‘digital front door’ for healthcare
<p><b>Assess your patients’ needs before tailoring apps and data for them.</b></p>
<p>If you work for a healthcare provider, you’ve probably heard rumblings from on high recently: The C-suite is eager to create something called a “digital front door” (DFD) that will supposedly make it easier and faster for patients to get the information they need.</p> <p>Without a detailed roadmap, or sometimes even a clear understanding of what a DFD is, IT leadership implements a DFD solution with glitzy features such as a chatbot. But once patients start using it, they find the new front door, which is supposed to improve their experience by simplifying it, leads to the same complex mix of applications and websites they struggled with before.</p>
#
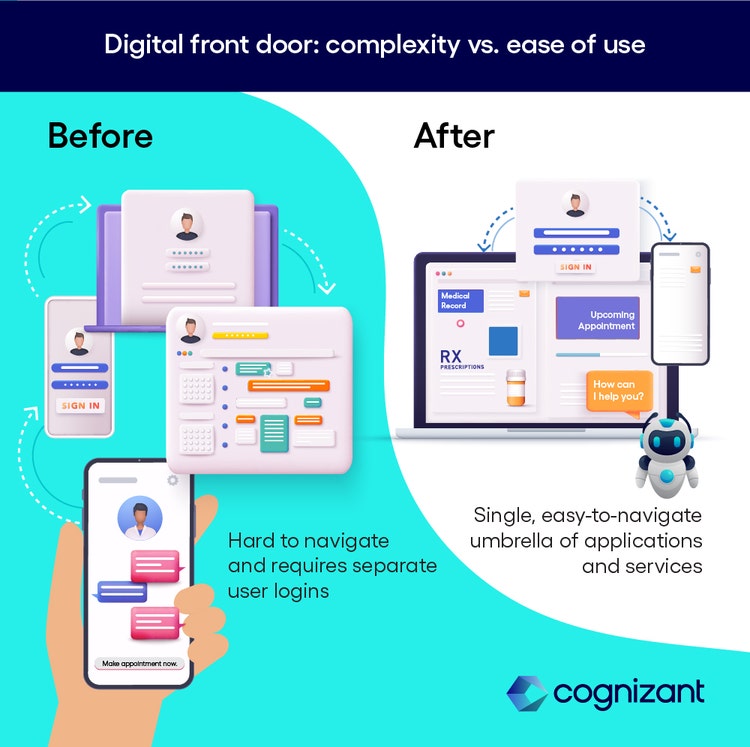
<p><span class="small">Figure 1</span></p> <p>Asking the chatbot to schedule an appointment, for example, might dump a user into a hard-to-navigate calendar that requires a separate login. Faced with such complexity, patients’ satisfaction scores sink further, and the health system must start over, having wasted time and money without fundamentally improving the patient experience.</p> <p>The most successful DFDs we’ve seen do more than just link to existing applications and web pages through a chatbot or create a new interface to the provider’s existing systems. They are instead tailored to the unique needs of each health system and their target patient population. They reflect a rethinking of each step in the patient experience to make the care process far easier and less stressful, increasing access to care and the quality of that care.</p> <p>For the patient scheduling an appointment, for example, the chatbot might tap the details of their upcoming visit and their past medical records to remind them to fast before a scheduled blood test, or to offer a ride.</p> <p>This up-front work, which can be done in as little as a few weeks, provides a solid foundation for a single, easy-to-navigate umbrella of applications and services that fundamentally transforms and enhances the patient experience.</p> <p>These are the eight steps we’ve found that are critical to DFD success.</p> <ol> <li><b>Define the patient’s needs.</b> Interview your customer support staff and review your support call logs to identify the most troublesome processes for patients. Then ask how you can improve them. Supplement this with focus groups asking patients which types of information would be most useful to them, and in which form. This helps ensure your DFD is optimized to their needs, whether they are digital-savvy patients using high-end concierge medical services or low-income Medicaid patients.<br> <br> </li> <li><b>Build out your technology landscape.</b> Identify the types of data and services your users need most, and where you lack the applications or infrastructure to deliver it. What would it take, for example, to make it easier for a patient to view their lab results, renew a prescription or schedule a telehealth appointment? What infrastructure would not only help meet each stand-alone need, but make it easy for the patient to move from one process to another without navigating different interfaces, creating a new account or reentering information?<br> <br> </li> <li><b>Create an intuitive launch pad </b>from which users can easily access these new improved workflows. This may be as simple as a new homepage on your website, with graphical icons linked to the most requested data or services, along with supporting content to help users understand each service. Think of this as your true digital front door—one that’s based on an understanding of the patient’s needs, with the underlying infrastructure to deliver a superior experience once they’re through the door.<br> <br> </li> <li><b>Enable single sign-on (SSO).</b> Enabling a user, once they have entered their username and password, to access any of the functions or data they need without creating or remembering other passwords, is one of the biggest improvements you can make to the user experience. It requires a single database of user information and authentication credentials and some modification of your apps. While you’re centralizing login, make changes so that all notifications from the various services (such as appointment reminders, billing notices, and prescription renewals) appear in a single location to improve the user experience.<br> <br> </li> <li><b>Link your apps.</b> Break the boundaries between applications. Deliver their capabilities to patients via SSO-enabled deep links directly to applications to eliminate the need to reenter usernames and passwords. Use these deep links to give patients the next information or form they need in an intuitive, easy-to-follow journey. Allow users to easily move from one application, database or service to another—for example, enable them to drill down into an electronic medical record from your billing app to understand what they’re being charged for. As you create this journey, test each step with patients to ensure it matches their behavior and needs.<br> <br> </li> <li><b>Make it conversational. </b>Use your deep understanding of users’ needs to provide an intuitive, empathetic, personalized interface and updates using technologies such as chatbots. Add a layer of conversational artificial intelligence (AI) to the launchpad; this will give patients the information they need or steer them to the next required step in easy-to-understand terms and may even perform that next step (such as opening an application) for them. Rather than asking patients to find the right functionality, present it to them based on their needs at each step in the journey.<br> <br> </li> <li><b>Pre-fill forms.</b> Use the application programming interfaces and other links you tapped in Step 5 to pre-fill common information (address, insurance coverage, medication lists, etc.) in forms patients must complete. This pre-filling could be triggered by such events as a request to schedule an appointment, and the patient must be allowed to approve the information before submitting it. This simple step can go a long way toward boosting satisfaction scores.<br> <br> </li> <li><b>Plan for future enhancements. </b>Investigate and begin deploying capabilities such as AI-powered personal health assistants that will allow you to provide personalized, proactive help to patients. (“We noticed you asked your primary care physician about weight loss medication and registered for but did not attend a weight management webinar. Would you like to schedule a confidential telehealth visit with one of our nutrition specialists?”)</li> </ol> <p>These steps take a bit more work upfront than grabbing a one-size-fits-all DFD solution, but they will save money and effort in the long run by eliminating the need to rip and replace your ineffective DFD when it makes life harder, rather than easier, for your patients. Better still, you’ll be able to report real increases in patient satisfaction to those impatient folks in the C-suite.</p> <p>To learn more, visit the <a href="https://www.cognizant.com/us/en/industries/healthcare-technology-solutions" target="_blank" rel="noopener noreferrer">Healthcare</a> section of our website or <a href="https://www.cognizant.com/us/en/about-cognizant/contact-us" target="_blank" rel="noopener noreferrer">contact us</a>.</p> <p><i>This article was written by Michael Wells, Senior Consultant, and Sahil Chaudhry, Consulting Manager, in Cognizant’s Healthcare practice.</i></p>
<p>We’re here to offer you practical and unique solutions to today’s most pressing technology challenges. Across industries and markets, get inspired today for success tomorrow.</p>
